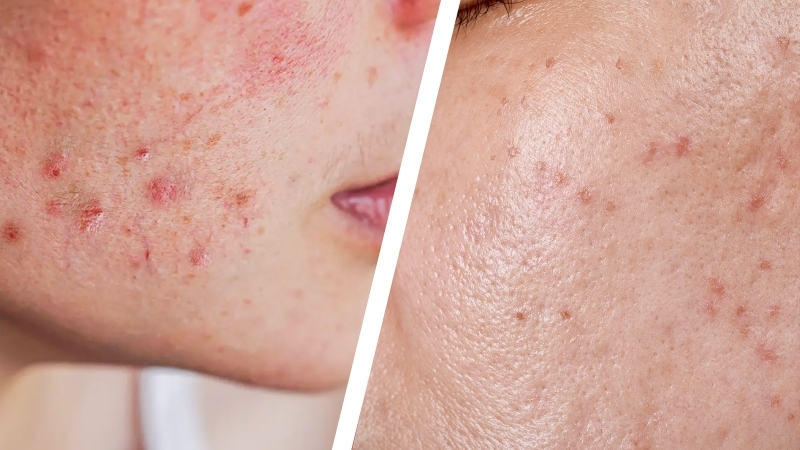
Regular acne happens when pores get clogged with oil, dead skin, and inflammation, often with bacteria also playing a role. Fungal acne, by contrast, involves an overgrowth of yeast in the hair follicles.
That difference matters because the two conditions can look similar at a glance, but they usually do not respond to the same treatment. Acne treatments like benzoyl peroxide, retinoids, or salicylic acid may help treat acne, while fungal folliculitis often needs antifungal treatment instead.
This is where many people get confused. They see small bumps on the forehead, chest, or back and assume it is acne.
But fungal acne often has a more uniform, itchy, rash-like appearance, while regular acne is usually more mixed, with blackheads, whiteheads, inflamed pimples, and sometimes deeper nodules all appearing together.
NCBI notes that Malassezia folliculitis is commonly mistaken for acne vulgaris because both can create acne-like bumps, but the underlying cause and best treatment are different.
Why People Mix Them Up So Often
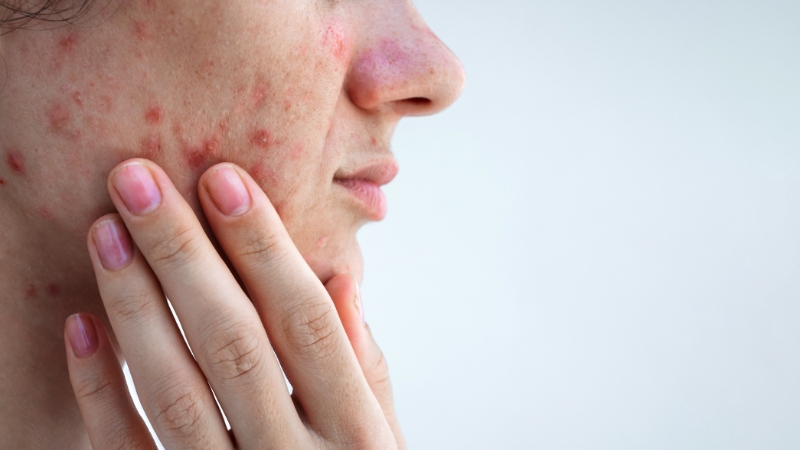
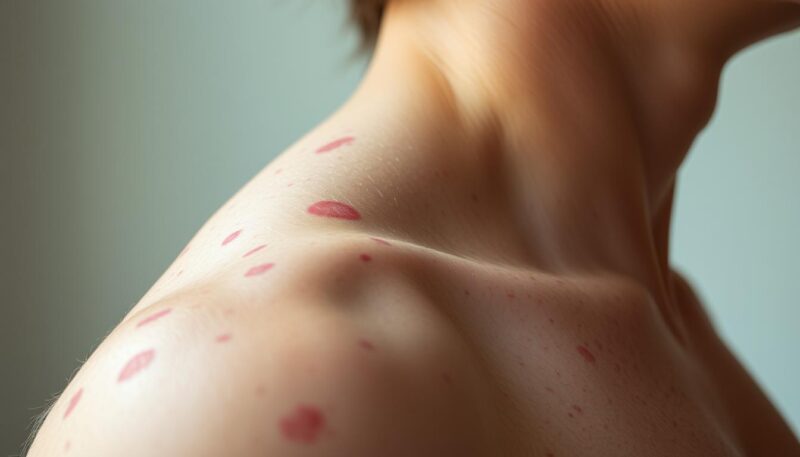
The main reason is visual overlap. Both conditions can show up as red bumps and pustules, especially in oily areas or in places where sweat builds up. On the face, chest, shoulders, and upper back, fungal folliculitis can easily look like a breakout.
DermNet specifically notes that diagnosis is often delayed because it resembles acne vulgaris and other kinds of folliculitis.
Another reason is that “fungal acne” is a popular online term, but it is not the formal name doctors use. The medical term matters because it reminds you that this is a folliculitis, meaning inflammation involving the hair follicles, not classic acne.
Cleveland Clinic and the American Academy of Dermatology both explain that the condition is caused by yeast overgrowth in follicles rather than the clogged-pore process that drives acne vulgaris.
What Regular Acne Actually Is
Regular acne, or acne vulgaris, is a very common skin condition in which hair follicles become blocked with oil and dead skin cells. Inflammation then contributes to the familiar mix of blackheads, whiteheads, papules, pustules, and in some cases deeper nodules or cysts.
Mayo Clinic describes acne as involving plugged hair follicles and notes that it commonly appears on the face, forehead, chest, upper back, and shoulders because these areas have more oil glands.
Acne often comes in different lesion types at the same time. Someone may have small clogged pores, a few red, inflamed pimples, and one or two more painful, deeper spots, all in the same area.
That mixed pattern is one clue that you may be dealing with acne rather than fungal folliculitis.
What Fungal Acne Actually Is
Fungal acne is usually Malassezia folliculitis, a condition caused by an overgrowth of Malassezia yeast in the hair follicles.
In plain language, it tends to appear as many small, similar-looking, inflamed bumps centered around follicles, often in areas that get warm, sweaty, and occluded.
It is often worse in hot, humid conditions, and can flare when skin stays sweaty, oily, or occluded for long periods.
The AAD notes that these bumps typically show up on the forehead, chest, and upper back, where there are many hair follicles, and that they can worsen in heat and humidity.
The Biggest Differences In Symptoms
One of the most useful clues is itching. Fungal acne is often itchy. Regular acne usually is not. Cleveland Clinic explicitly highlights itch as one of the main differences between the two.
That does not mean every itchy bump is fungal folliculitis, but if the bumps are very similar in size and the area feels itchy more than sore, fungal folliculitis becomes more likely.
Another difference is uniformity. Fungal acne often looks more monomorphic, meaning the bumps tend to be similar in size and shape.
Regular acne is usually more mixed. You might see blackheads, whiteheads, inflamed pimples, and healing marks all at once.
Symptom Comparison Table
Feature
Fungal Acne
Regular Acne
Main process
Yeast overgrowth in hair follicles
Clogged follicles with oil, dead skin, and inflammation
Itching
Common
Usually not a major feature
Lesion pattern
Many similar-looking bumps
Mixed lesion types
Blackheads or whiteheads
Usually absent
Common
Common locations
Forehead, chest, upper back, shoulders
Face, forehead, chest, back, shoulders
Common triggers
Heat, humidity, sweat, occlusion
Hormones, oil production, pore clogging, and inflammation
Best treatment approach
Antifungal treatment
Acne-directed treatment
This table is a practical shortcut, but it is still not a substitute for an actual diagnosis because bacterial folliculitis, steroid acne, and other conditions can also resemble both. DermNet specifically lists acne vulgaris, steroid acne, and bacterial folliculitis in the differential diagnosis.
How The Bumps Usually Look
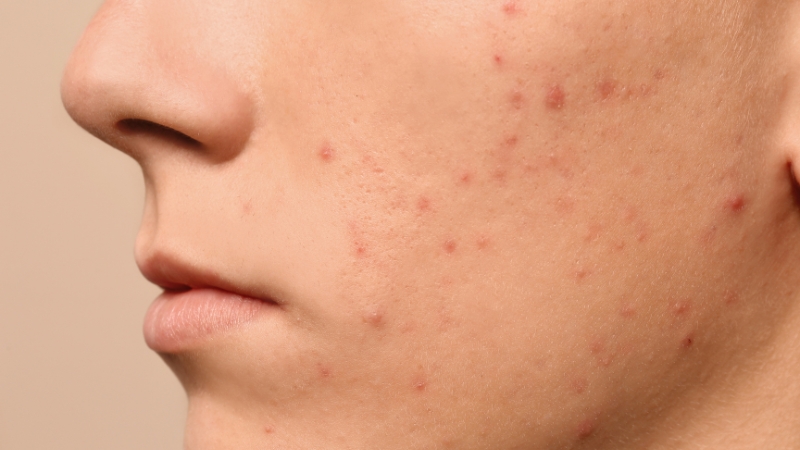
Fungal acne often appears as clusters of small red bumps or pustules that look very similar to one another. Many people describe it as a “rash of tiny pimples.”
Regular acne is more visually varied. It may include blackheads, closed comedones, inflamed red pimples, pus-filled spots, and, in more severe cases, deeper painful nodules.
Visual Pattern Table
Visual Clue
More Suggestive Of Fungal Acne
More Suggestive Of Regular Acne
Tiny bumps that all look alike
Yes
Less typical
Blackheads around the area
No
Yes
Deep, painful cyst-like spots
Uncommon
More consistent with inflammatory acne
Itchy rash-like clusters
Yes
Less typical
Mixed old and new lesion types
Less typical
Common
A lot of people online use “fungal acne” to describe any small forehead bumps, but that is too broad. Small forehead bumps can also be comedonal acne, irritation, bacterial folliculitis, or product-related breakouts.
Where Each One Usually Shows Up
Both conditions can affect the face and upper body, which is another reason they get confused. But fungal acne often shows up on the forehead, chest, shoulders, and upper back, especially in sweaty or humid conditions.
These areas tend to have a lot of follicles and are often exposed to heat, occlusion, or friction.
Regular acne also commonly appears on the face, forehead, chest, upper back, and shoulders, but it is especially associated with oil-rich areas and can appear in a more classic “teen or adult acne” pattern across the face and jawline, depending on the person.
What Tends To Trigger Fungal Acne
View this post on Instagram
Fungal acne often becomes more likely when the skin environment favors yeast overgrowth. Heat, sweating, humidity, tight clothing, heavy occlusion, and sometimes recent antibiotic use can shift the balance.
DermNet specifically notes that treatment may involve stopping antibiotics and avoiding moisturizers in affected areas, which reflects how the condition can be encouraged by skin environments that trap heat and oil.
This does not mean antibiotics always cause fungal folliculitis, but it is a recognized pattern because antibiotics can reduce competing bacteria and change the skin environment.
That is one reason why a breakout that seems to worsen during acne antibiotic treatment can sometimes turn out not to be acne at all.
This is an inference supported by dermatology sources discussing the role of antibiotics and differential diagnosis.
What Tends To Trigger Regular Acne
Acne is more strongly linked with oil production, clogged follicles, hormonal shifts, inflammation, and sometimes family history.
That is why regular acne often flares around puberty, menstrual hormone changes, stress-related routines, occlusive cosmetics, or heavy hair and skin products. Those triggers do not rule out fungal folliculitis, but they fit more naturally into the acne picture.
Why Treatment Often Fails When The Diagnosis Is Wrong
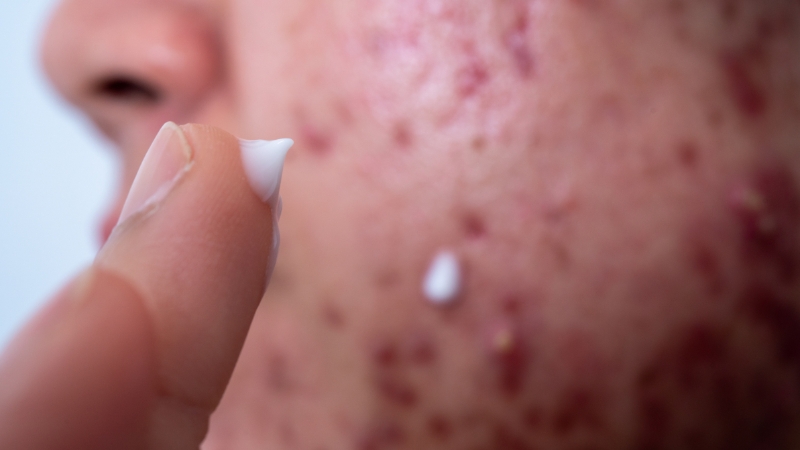
This is one of the most important practical differences. If someone has true acne and only uses antifungal products, improvement may be limited.
But if they have fungal folliculitis and keep using acne antibiotics alone, or keep layering occlusive products while assuming it is standard acne, the condition may persist or worsen.
DermNet also notes that Malassezia folliculitis may be treated with topical antifungals or oral antifungals, while ordinary acne therapy is a separate treatment pathway.
How Fungal Acne Is Usually Treated
Fungal acne is generally treated with antifungal therapy, not classic acne treatment alone. Cleveland Clinic notes that topical antifungal creams and sometimes oral antifungal medications are used. DermNet similarly describes topical or oral antifungal treatment for Malassezia folliculitis.
Supportive measures often include reducing sweat buildup, changing out of damp clothing promptly, and avoiding very occlusive products in affected areas.
Those measures do not replace treatment, but they can help reduce the skin conditions that favor yeast overgrowth.
This is consistent with DermNet’s advice about avoiding moisturizers and adjusting contributing factors.
How Regular Acne Is Usually Treated
@dra_says Acne, i think we are doing it wrong! #acne #spots #skin #oilyskin #roaccuatane #dermatology #fibromyalgia #stress #anxiety #cysts #skinproblem #acnecauses #benzoylperoxide #dryskin #acnecream #chronicfatigue ♬ original sound – Dr Ahmed
Regular acne treatment depends on the type and severity of lesions. Mild acne may respond to over-the-counter ingredients such as benzoyl peroxide, salicylic acid, or adapalene, while more persistent or inflammatory acne may require prescription retinoids, antibiotics, hormonal therapy, or isotretinoin in severe cases.
That is why using the right category of treatment matters. A comedonal acne breakout with blackheads and whiteheads will not usually clear with antifungal treatment alone, because the core issue is clogged follicles, not yeast overgrowth.
Treatment Direction Table
Condition
Typical First-Line Direction
What Often Does Not Help Enough By Itself
Fungal acne
Topical or oral antifungal treatment
Acne-only routines that ignore yeast involvement
Regular acne
Benzoyl peroxide, retinoids, salicylic acid, and other acne therapies based on severity
Antifungal treatment alone
Unclear rash-like bumps
Clinical evaluation, sometimes testing
Self-diagnosing from photos alone
If the pattern is unclear, the safest route is not to keep cycling through random products. A dermatologist can often tell the difference clinically and may use testing when needed.
Can You Have Both At The Same Time?
Yes, that can happen. A person can have underlying acne-prone skin and also develop Malassezia folliculitis, especially if heat, sweat, occlusion, or recent antibiotic use changes the skin environment.
Dermatology sources emphasize that the resemblance between the conditions can complicate diagnosis, which also implies that overlap is possible in real patients.
This is one reason treatment can feel confusing. Someone may improve partly with acne treatment but still have a stubborn, itchy, uniform breakout on the forehead or trunk that turns out to be fungal folliculitis layered on top of acne.
That is an inference from the documented overlap and differential diagnosis, not a stand-alone diagnostic rule.
When Is It More Likely To Be Fungal Acne
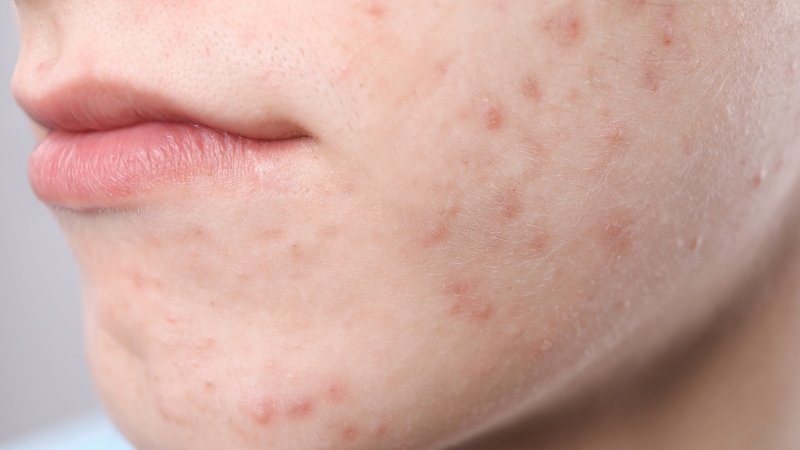
A fungal pattern becomes more likely when the bumps are very similar to each other, the area is itchy, the breakout is concentrated on the forehead, chest, shoulders, or upper back, and the skin has been exposed to heat, humidity, sweat, or occlusive clothing.
It is also worth considering when someone has not improved with typical acne treatment, especially if the rash seems to worsen under conditions that favor yeast.
When It Is More Likely To Be Regular Acne
A regular acne pattern becomes more likely when there are blackheads and whiteheads, when lesions are mixed in type rather than uniform, when there are deeper, inflamed nodules or cysts, and when the breakout follows a familiar acne pattern over time.
Mayo Clinic’s description of acne supports this more varied lesion pattern.
When To See A Dermatologist
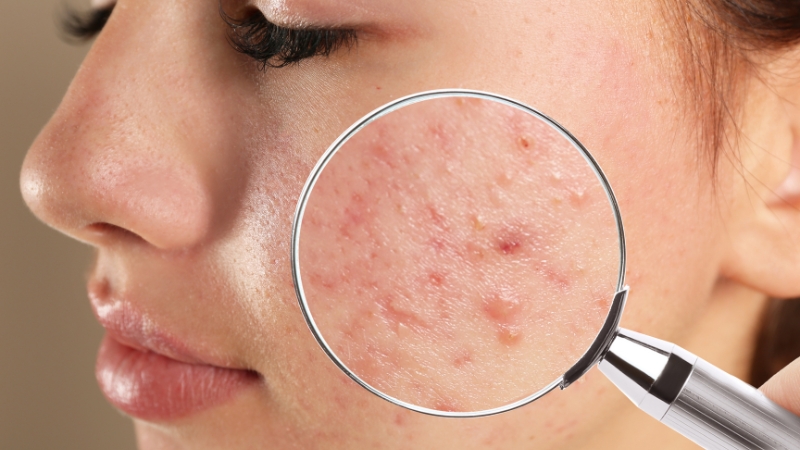
A dermatologist visit is a good idea when breakouts are persistent, very inflamed, itchy, and unusual, leaving marks, or not responding to what should be the right treatment.
It is also worth getting checked when you are unsure whether you are dealing with acne, fungal folliculitis, or another lookalike condition, such as bacterial folliculitis, steroid acne, or hidradenitis in body-fold areas.
Bottom Line
The difference between fungal acne and regular acne comes down to cause, pattern, and treatment.
Fungal acne is usually Malassezia folliculitis, a yeast-related inflammation of hair follicles that often causes itchy, uniform bumps on the forehead, chest, shoulders, or back.
Regular acne is a clogged-follicle inflammatory skin condition that more often shows a mixed pattern of blackheads, whiteheads, pimples, and sometimes deeper lesions.
They can look similar, but they are not the same condition, and treating the wrong one is a common reason breakouts drag on.