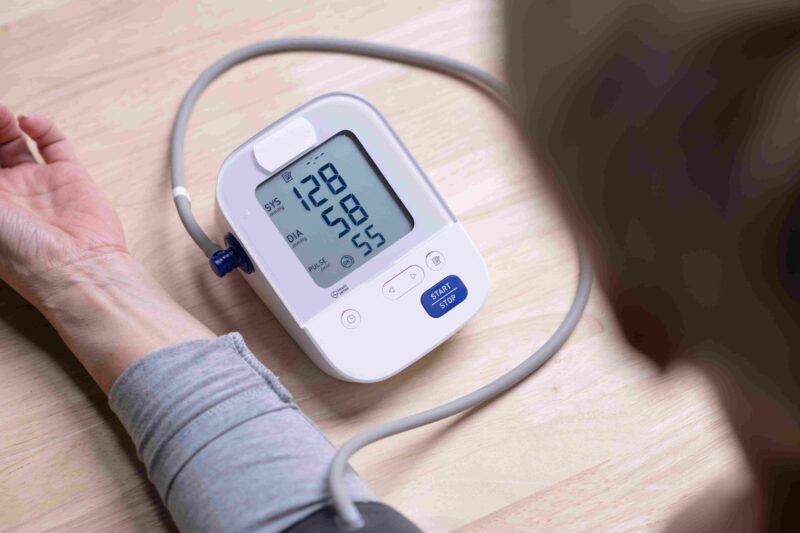
Monitoring blood pressure at home plays an important role in long-term health management. Regular checks allow early detection of hypertension and can reveal masked hypertension, a condition where readings appear normal in a clinical setting but remain elevated at home.
Consistent home measurements also help track how well treatment is working over time. Readings taken in a familiar environment reduce the “white coat” effect, which can cause higher values during medical visits due to anxiety.
Home monitoring is often recommended for people diagnosed with high blood pressure, those starting or adjusting medication, and individuals with increased cardiovascular risk.
Reliable tracking supports better decisions and helps prevent complications.
Choosing the Right Equipment
Accurate home blood pressure monitoring begins with device choice, which directly affects the quality of readings, which in turn influences medical decisions and long-term health management. Careful selection reduces the risk of inaccurate measurements and unnecessary concern.
A validated, automatic upper-arm blood pressure monitor is strongly recommended.
Upper-arm devices provide more consistent and dependable results compared to wrist or finger monitors. Wrist and finger devices are more sensitive to body position and often produce inconsistent values if not used precisely.
Cuff size plays a critical role in accuracy. Incorrect sizing can lead to readings that are either too high or too low. The cuff bladder should cover about 80% of the arm circumference, ensuring proper compression of the artery.
Measuring arm circumference helps determine the correct cuff size. Measurement should be taken midway between the shoulder and the elbow while the arm is relaxed. Many monitors offer different cuff sizes, so matching the cuff to arm size is essential.
Advanced features can improve convenience and consistency.
Regular accuracy checks help maintain confidence in readings. Bringing the monitor to a medical appointment allows direct comparison with a professional device. Small differences may occur, but large discrepancies should be addressed to ensure reliable performance.

Preparing for Measurement
Preparation has a direct impact on reading accuracy. Small actions taken before measurement can significantly influence blood pressure values. Consistent preparation habits help produce stable and comparable results over time.
- Caffeine intake
- Smoking
- Alcohol consumption
- Physical exercise
Each of these can temporarily raise blood pressure and distort results.
Bladder condition also affects readings. Emptying the bladder before measurement helps avoid artificially elevated values. Resting quietly for at least five minutes allows the body to return to a baseline state, which improves consistency.
The environment plays an important role. Measurements should be taken in a quiet, comfortable space without distractions. Stress, noise, or discomfort can influence results and reduce reliability.
Certain situations should be avoided when measuring blood pressure. Examples include times of emotional stress, exposure to cold temperatures, or immediately after waking without resting. Calm and stable conditions support accurate measurement.
Correct Body Position

Body position directly affects blood pressure readings. Even small deviations can lead to noticeable differences in results. Proper posture ensures that measurements reflect true cardiovascular status.
Seated posture should follow specific guidelines. The back should be supported by a chair, helping maintain a relaxed position. Feet must remain flat on the floor, with legs uncrossed to prevent changes in circulation.
Arm positioning is equally important. The arm should rest on a stable, flat surface, such as a table. The upper arm must be positioned at heart level to avoid artificially high or low readings.
Proper placement of the cuff ensures effective measurement.
- Place the cuff directly on bare skin, not over clothing
- Align the cuff with the artery, using the marker provided on most devices
- Position the lower edge of the cuff about 2 centimeters above the elbow
Movement and speech can interfere with measurement. Remaining still and silent during the reading helps maintain accuracy and prevents fluctuations.
Proper Measurement Technique
Consistent technique ensures reliable results across multiple readings. Small variations in method can lead to inconsistent values, making it harder to track trends over time.
Cuff application should be firm but comfortable. Tightness should allow one finger to fit underneath the cuff, ensuring proper pressure without excessive constriction. Device instructions should always be followed closely for correct operation.
Multiple readings improve accuracy. At least two measurements should be taken, with a one to two-minute pause between them. If values differ significantly, additional readings should be taken and averaged for a more accurate result.
Daily timing should remain consistent. Maintaining a routine helps reduce variability caused by natural fluctuations throughout the day.
Initial monitoring requires more frequent measurements. Readings should be taken twice daily for at least four to seven days. First-day results may be excluded if advised by a healthcare provider, as early readings can be less stable.
Certain practices should be avoided to maintain accuracy. Measuring over clothing or immediately after physical activity can distort results and should be avoided whenever possible.

Recording and Tracking Results
Accurate record keeping transforms individual readings into meaningful data. Tracking results over time allows patterns to emerge, which supports better health decisions and communication with healthcare providers.
Each recorded entry should include essential details.
- Date and time of measurement
- Systolic value, representing the top number
- Diastolic value, representing the bottom number
- Notes about stress, symptoms, or missed medication
Multiple methods can be used to maintain records. Options include handwritten logs, digital applications, or built-in monitor memory. Consistency matters more than the format used.
Averaging readings over several days provides a more reliable picture than relying on a single measurement.
Bringing both the log and the monitor to medical appointments allows healthcare providers to review patterns and verify device accuracy. Regular review supports better diagnosis, treatment adjustments, and long-term health management.
Summary
Home blood pressure monitoring provides reliable and clinically recommended data when performed correctly. Accuracy depends on proper preparation, correct positioning, and consistent measurement habits.
Regular tracking supports improved diagnosis, more effective treatment adjustments, and reduced long-term cardiovascular risk.